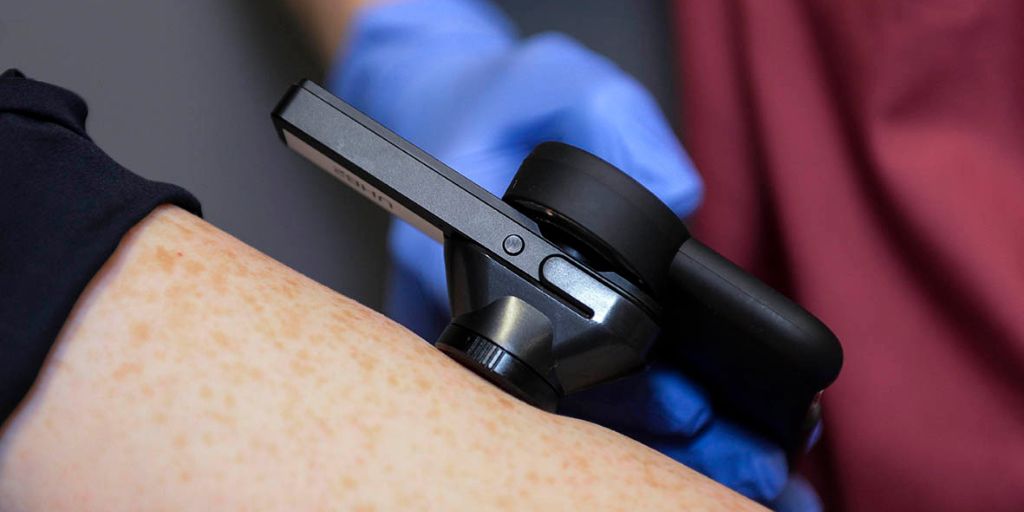
People in North Lancashire and South Cumbria who have suspected skin cancer are to benefit from faster diagnosis thanks to ground-breaking new technology at University Hospitals of Morecambe Bay Trust (UHMBT).
The pilot program with medical technology company Skin Analytics, combines AI (artificial intelligence) technology and teledermoscopy to diagnose and treat people with skin cancer, earlier.
The programme has been made possible thanks to funding from the Lancashire and South Cumbria Cancer Alliance. The technologies are set to significantly speed up the patient’s journey from referral to the service for suspected skin cancer, to diagnosis and, if necessary, treatment.
In the pilot, a healthcare assistant will take a high-quality image of the patient’s suspected cancerous skin lesion in a procedure called teledermoscopy. The AI technology, called DERM will then analyse the image of the skin lesion, supporting the decision of whether the patient needs to be seen in a face-to-face clinic for further examination.
The combination of technologies will enable clinicians to review more suspected cancer cases in a shorter space of time. This will mean faster treatment for patients with skin cancer and avoid unnecessary hospital appointments for those who don’t.
Dr Robert Burd, consultant dermatology and lead for dermatology at UHMBT, said: “With the rate of skin cancer rising at UHMBT, our mission is clear: we need to explore better digital solutions to fast-track skin cancer diagnoses and effectively manage our dermatology resources. Ultimately, our goal is to reduce patient wait times and ensure timely interventions. Everyone, whether suspected of cancer or not, deserves prompt and efficient care.”
Neil Daly, CEO of Skin Analytics, added: “Our driving passion has always been to make a tangible difference in people’s lives. DERM, for us, is more than just technology, it’s a tool that finds the ‘needle in the haystack.’ It acts as a triaging system, ensuring that patients with malignant lesions receive prioritised attention and a face-to-face consultation with a dermatologist.”
Patients referred to either Royal Lancaster Infirmary or Furness General Hospital for suspected skin cancer will benefit from the new pathway.
Melanoma is the fifth most common cancer in the UK, and has seen incidence rates double since 1990 [according to the charity Melanoma UK].
Cancer Research UK also predicts that by 2040, skin cancer cases will rise by 50%, reaching up to 26,500 annually. It is thought that this increase is attributed to the boom in affordable package holidays during the 1960s.
DERM is already used in 13 NHS trusts and has helped more than 67,000 NHS patients and detected more than 5,300 cancer cases across the UK to date. It uses machine learning and AI image analysis technology to identify cancerous lesions. Performance has been evaluated in clinical trials and real-world deployments, demonstrating DERM can identify melanoma and NMSC (SCC and BCC) with similar accuracy to dermatologists whilst also identifying seven out of every 10 benign lesions that do not require specialist input. This can help to increase trust capacity and reduce service pressure, freeing up consultant dermatologist time to be spent with the patients who need them most.