By Phil Norris, Head of Marketing and Analytics, VirtaMed
Training healthcare professionals is clearly important in any scenario. Medical education provides us with the nurses, doctors and surgeons of the future. The coronavirus pandemic has meant that the global healthcare community has shifted its focus on emergency care rather than education – for painfully obvious reasons.
Due to Coronavirus, many elective procedures have been cancelled and the contact between healthcare professionals and patients has been restricted. As medical procedures are taught in an apprenticeship model, many trainees are now left without the ability to train. Moreover, once the COVID restrictions are relaxed, there will be a backlog of exams and elective procedures to be done, which will reduce available training opportunities. There has been an additional strain placed on the provision of medical professionals due to the shortage of PPE. Many hospitals have cancelled clinical rotations for medical residents to preserve PPE for caregivers and safeguard students and patients. Students have expressed concerns that they will not complete their required clinical hours in time to graduate this year, and the pipeline of new medical professionals could be reduced when they are most needed. So how can MedTech rise to the challenge?
Simulation Technologies
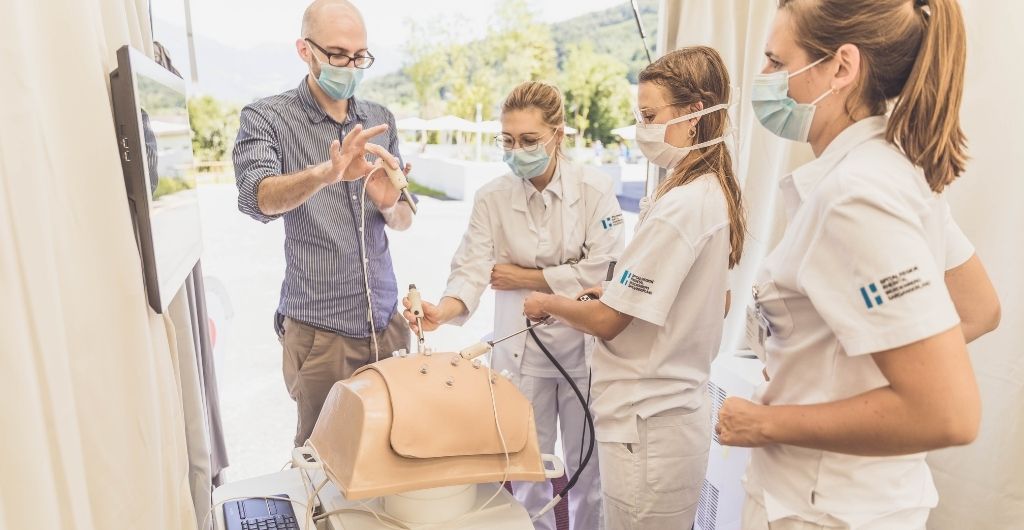
High fidelity simulators provide an environment to gain medical skills and practice procedures, enhanced by automated real-time validated performance feedback. Even under COVID restrictions, physicians can safely practice surgical procedures in a simulated environment and ensure that they continue improving their core skills. Simulators reduce costs for disposable material during physician training; also, equipment breakage costs can be reduced significantly. Aside from the obvious social distancing advantages that working with simulators provides, where else are we seeing benefits under COVID conditions? Simulation technologies are available across a variety of surgical specialties including Gynecology and Obstetrics, Orthopedic, Arthroscopy and more. Simulators such as Virtamed’s LaparoS are being utilised across a variety of medical training institutions. Users of simulators are finding that the surgical training outcomes are greatly improved which in turns supports better patient care.
Efficient redeployment of medical staff
With some medical staff, either furloughed or in a high-risk group and encouraged not to go to the hospital currently due to COVID, they are in a position to invest more time to provide input to future courses. Some of these experts are able to give their advice to simulator design in the continuing quest to develop and enhance simulators across different disciplines. Also, they are able to share their knowledge, presenting their published academic work by webinar accompanied by illustrative procedures on the simulator – perfect for these current lockdown conditions. In a similar vein, retired medical staff or those nearing retirement have fewer commitments anyway and can help with advice/course design. Those in previous medical positions are using their breadth of knowledge and experiences to be part of the development of future medical technologies.
Cost savings
While healthcare systems, in general, are under huge financial pressures, any way to save money is a boon. Is training via simulators cheaper than being taught using traditional methods?
Many training costs are deeply ingrained into our healthcare systems, but some studies have brought the implicit costs to light. By pre-training a certain set of skills up to a defined level on simulators, residents can operate with more precision and greater speed, improving the efficiency of the clinical schedule. Pre-training also means that professors can dedicate their time to sharing their advanced knowledge, reducing the time spent on the basics. These efficiencies, combined with a reduction in cadaveric courses and the corresponding reduction in the use of disposables and instrument breakages, mean that a typical teaching institution improves their standard of training and reduces costs within 2-3 years of adopting simulation.
A fast track to the medical future?
Will the pandemic provide a fundamental shift in training (using simulators) in the same way that, for example, grounded pilots are currently spending a lot of time in simulators in order to keep their logged hours up and maintain their qualifications? Is this the opportunity to fast-track some of that MedTech in our healthcare systems? Again, yes. Many medical societies have already made public statements about the need for simulation in lieu of elective procedures. Many university hospitals have teaching facilities (simulation centres) outside of their surgical building, which can be visited by surgeons in training. The longer-term outlook is how medical device companies can best connect with surgeons for training; shipping a simulator and delivering virtual training is a great alternative, especially if the original surgical instruments are incorporated into the simulation and the training data is remotely accessible.
Post COVID backlog
The huge backlog of patients that have accumulated through the cancellation of elective procedures will keep operating rooms at capacity into 2021. Therefore the emphasis must be for trainees to have independent learning tools available so that they can learn on-demand while still benefiting from performance feedback. High fidelity simulation is key to this. These simulators have codified a huge amount of medical expertise and can be relied upon to deliver the same standard of training over and over. And it’s much safer to practice on a simulator.











